Housing Insecurity Is Associated With Loss To Follow Up After Revascularization For Chronic Limb Threatening Ischemia
*Thomas Mcnamara BS, *Max Zhu , *Diana Rodriguez , *Nkiruka Arinze , *Thomas Cheng , Alik Farber , *Elizabeth King MD, *Andrea Alonso MD, Jeffrey Siracuse MD, MBA
Surgery, Boston University, Chobanian and Avedisian School of Medicine, Boston, MA
Background:
Adverse social determinants of health (SDH) have been associated with unfavorable surgical outcomes. However, housing insecurity has been poorly characterized, especially in the context of peripheral artery disease. Our goal was to evaluate housing insecurity and associated outcomes in patients undergoing lower extremity revascularization for chronic limb threatening ischemia (CLTI).
Study Design:
A single-center, retrospective chart review was performed at a safety-net hospital between 2017-2022 for patients undergoing lower extremity revascularization for CLTI who completed a SDH survey. Patients were categorized as housing insecure if they indicated unstable housing within one year of their procedure. Short and long-term outcomes were assessed by risk-adjusted analysis.
Results:
Of 320 patients (mean age 67 years, 57% male, 54% of Black race) who were analyzed, 83% experienced lower extremity tissue loss. The distribution of Wound, Ischemia, and foot Infection (WIfI) stages were as follows: 1 (11%), 2 (23%), 3 (31%), and 4 (35%). Endovascular, surgical and hybrid revascularization procedures were performed in 63%, 30%, and 7% of patients, respectively. Housing insecurity was reported by 13% of patients. On multivariable analysis, current tobacco use (OR 55, 95% CI 5.4-560, P=.001) and coronary artery disease (OR 3.1, 95% CI 1.1-8.5, p=.03) were independently associated with housing insecurity.
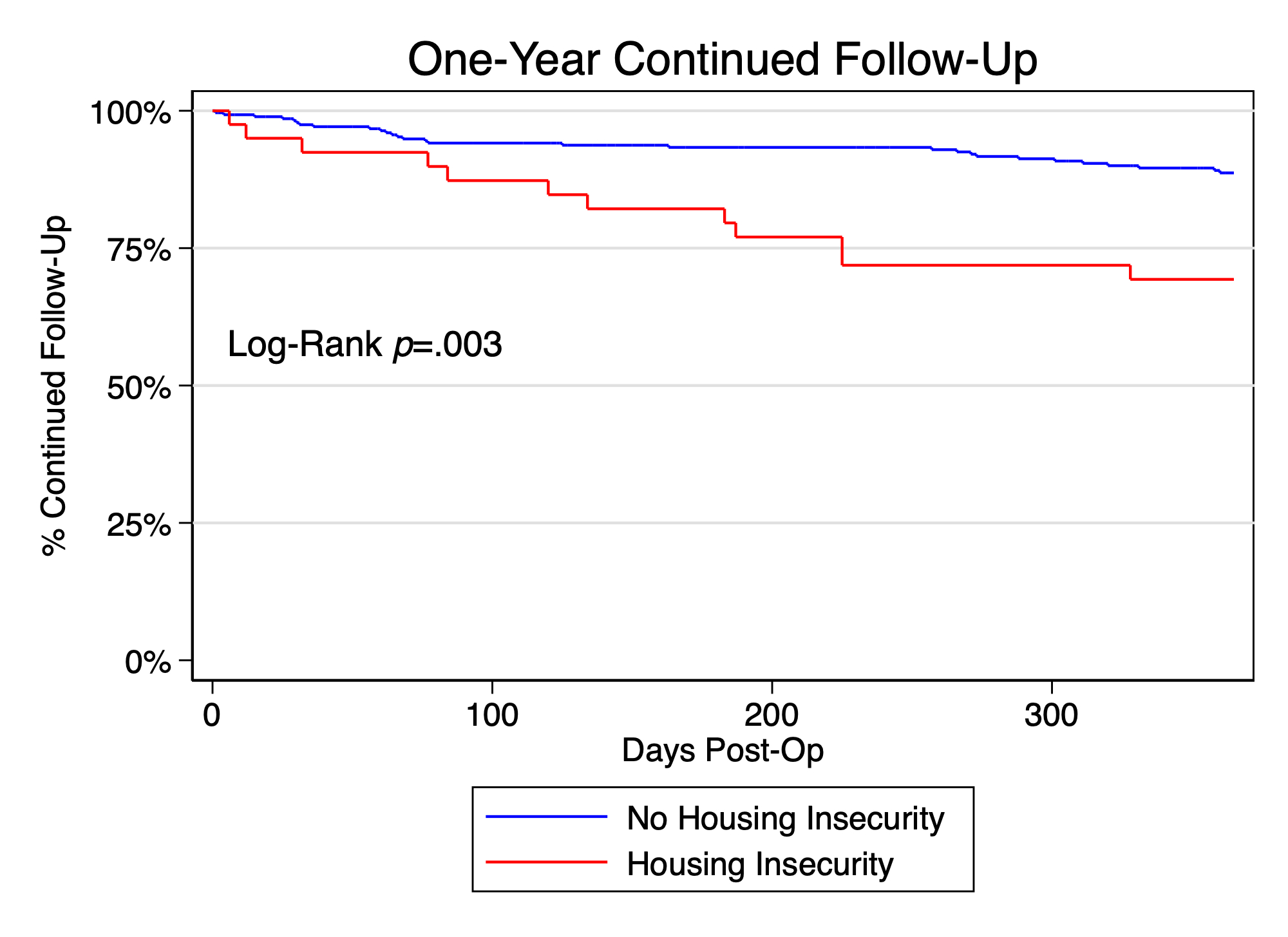
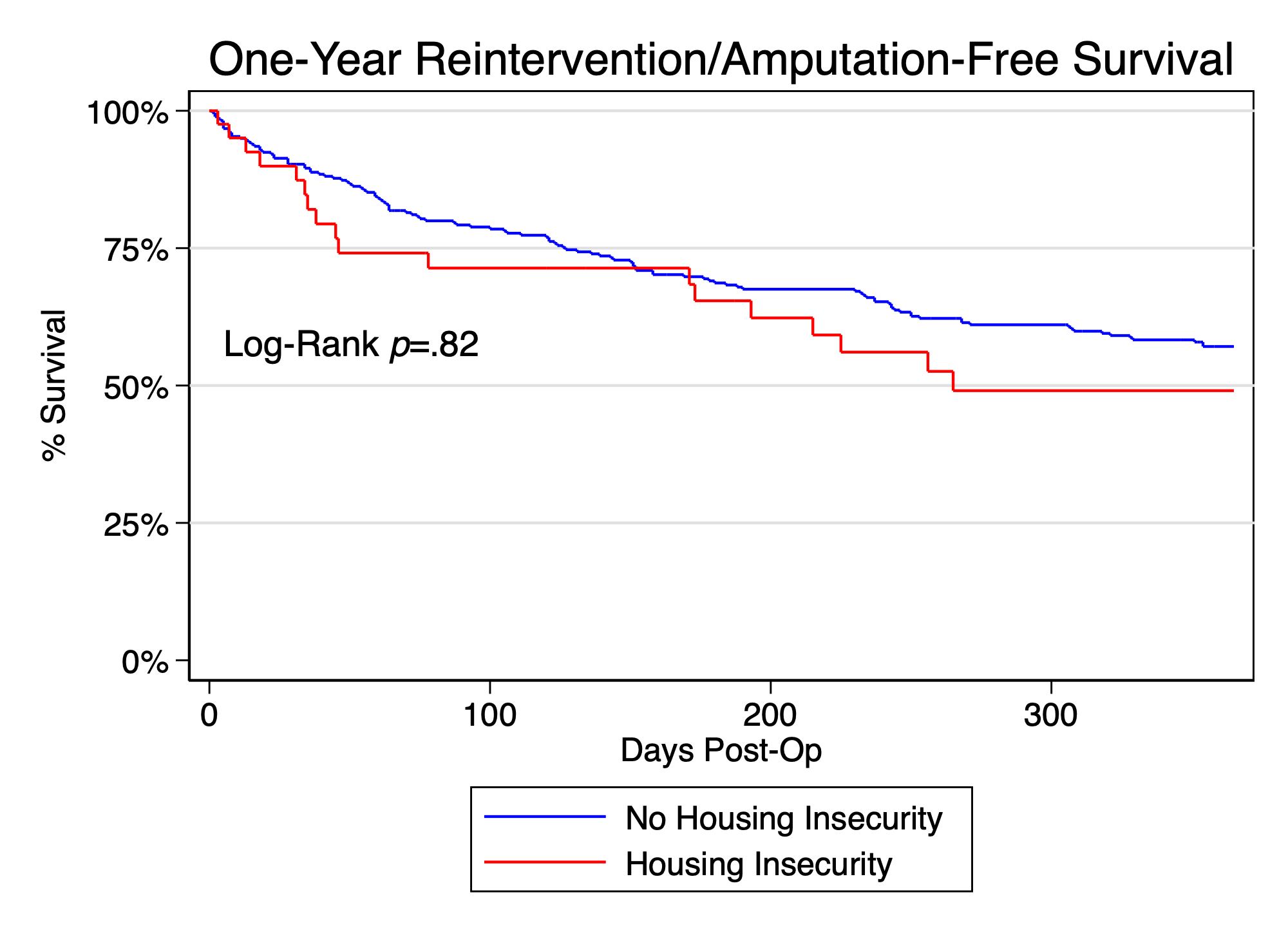
Patients with and without housing insecurity experienced similar rates of 90-day Emergency Department visits (61% vs 49%, P=.14) and readmissions (47% vs 46%, P=.39). Risk adjusted analysis showed that housing insecurity did not affect amputation rates (HR 1.6, 95% CI .86-2.9, p=.14) or major adverse limb events (MALE, HR 1.4, 95% CI .81-2.3, p=.24). Kaplan Meier analysis at 1-year indicated that patients with and without housing insecurity had similar rates of survival (.90 vs .82 p=.067), but patients with housing insecurity had lower rates of follow-up at 1-year (.69 vs .88, p=.003), which remained significant on risk adjusted analysis (HR 2.7, 95% CI 1.4-5.3, p=.005).
Conclusions:
Housing insecurity is common in the CLTI patient population. Patients with and without housing insecurity experienced similar rates of perioperative and one year amputation and survival outcomes. However, housing insecurity was associated with loss to follow-up within 1 year. SDH challenges should be screened and addressed in patients with CLTI undergoing surgery to potentially limit patient loss to follow-up.
Back to 2024 Abstracts


