The limited utility of preoperative hypoalbuminemia as an independent predictor of post-conversion and revisional bariatric surgery outcomes: an MBSAQIP registry analysis
*Pourya Medhati 1, *Jerry Dang MD PhD2, Eric Sheu 1, Ali Tavakkoli 1, Abdelrahman Nimeri 1, *Thomas Shin MD1
1Surgery, Brigham and Women's Hospital, Boston, MA; 2Cleveland Clinic, Cleveland, OH
Background: Anastomotic conversions and revisions remain crucial in addressing complications or sub-optimal outcomes following bariatric procedures. Preoperative malnutrition, proxied by hypoalbuminemia, has traditionally been considered a risk factor for postoperative morbidity. This study investigates the validity of this relationship in revisional and conversion bariatric surgery. Study Design: We conducted a retrospective cohort study of 58,327 bariatric revisions and anastomotic conversions from the 2020-2022 MBSAQIP registry and divided patients into two groups using a threshold preoperative albumin level of 3.5 g/dL. Nearly all cases studied were performed laparoscopically (98.8%). Descriptive statistics, multivariable logistic regression, and 1:1 nearest neighbor matching were used in complete-case analyses to assess the association between albumin levels and postoperative outcomes. Results: While univariate analyses demonstrate an association between hypoalbuminemia and postoperative morbidity, multivariable modeling showed hypoalbuminemia is not an independently significant driver of 30-day postoperative complications (OR 1.35, p=0.124), reoperation (OR 1.05, p=0.874), reintervention (OR 0.87, p=0.721), or readmissions (OR 1.30, p=0.212; Figure 1). Furthermore, 1:1 nearest neighbor match propensity analysis redemonstrates low albumin (< 3.5g/dL) does not significantly predict 30-day postoperative complications (OR 1.09, p=0.723), reoperations (OR 0.70, p=0.347), or reinterventions (OR 0.81, p=0.651). Propensity analysis did, however, yield significantly increased odds of 30-day postoperative readmission with low albumin (OR 1.75, p=0.045). Conclusions: Adjusting for confounding patient factors, hypoalbuminemia alone did not emerge as an independent predictive factor for the 30-day complications, reoperation, or re-intervention after revisional and anastomotic conversion bariatric surgery.
Table 1. Characteristics of patients undergoing revisions based on albumin levels
| Albumin ? 3.5 g/dL (n = 55,004) | Albumin < 3.5 g/dL (n = 3,323) | |
| Female* | 48,870 (88.9) | 3,038 (91.4) |
| Age, y, median (IQR) | 48.0 (40-55) | 48.1 (40-55) |
| BMI, median (IQR)* | 40.7 (35.3-45.3) | 41.3 (34.6-47.9) |
| Race* | ||
| White | 35,418 (64.4) | 1,882 (56.6) |
| Black | 13,017 (23.7) | 115 (33.6) |
| Hispanic* | 7,617 (15.2) | 401 (13.2) |
| Pre-procedure functional status* | ||
| Independent | 54,685 (99.5) | 3,268 (98.6) |
| Partially dependent | 259 (0.47) | 39 (1.2) |
| Totally dependent | 13 (0.02) | 6 (0.18) |
| American Society of Anesthesiology (ASA) Class* | ||
| ASA class I-II | 14,080 (25.7) | 696 (21.0) |
| ASA class III | 39,466 (71.9) | 2,437 (73.4) |
| ASA class IV | 1341 (2.4) | 188 (5.7) |
| Diabetes Mellitus* | 7,568 (13.8) | 523 (16) |
| Hypertension | 5,681 (38.5) | 393 (38.6) |
| Gastroesophageal reflux disease | 32,280 (58.7) | 1,927 (58) |
| Chronic obstructive pulmonary disease* | 617 (1.1) | 59 (1.8) |
| Anemia* | 22,054 (40.1) | 1,204 (36.2) |
| Hyperlipidemia | 10,401 (18.9) | 611 (18.4) |
| Renal insufficiency* | 192 (0.4) | 50 (1.5) |
| Dialysis use* | 78 (0.1) | 24 (0.7) |
| History venous thromboembolism* | 1,930 (3.5) | 209 (6.3) |
| History deep venous thrombosis* | 1,280 (2.3) | 155 (4.7) |
| History pulmonary embolus* | 1,055 (1.9) | 1,806 (3.3) |
| Therapeutic anticoagulation use* | 1,806 (3.3) | 190 (5.7) |
| Obstructive sleep apnea | 13,833 (25.2) | 767 (23.1) |
| Smoking history* | 2,670 (4.9) | 233 (7) |
* P<0.05. All data are presented as n (percentage) unless otherwise stated.
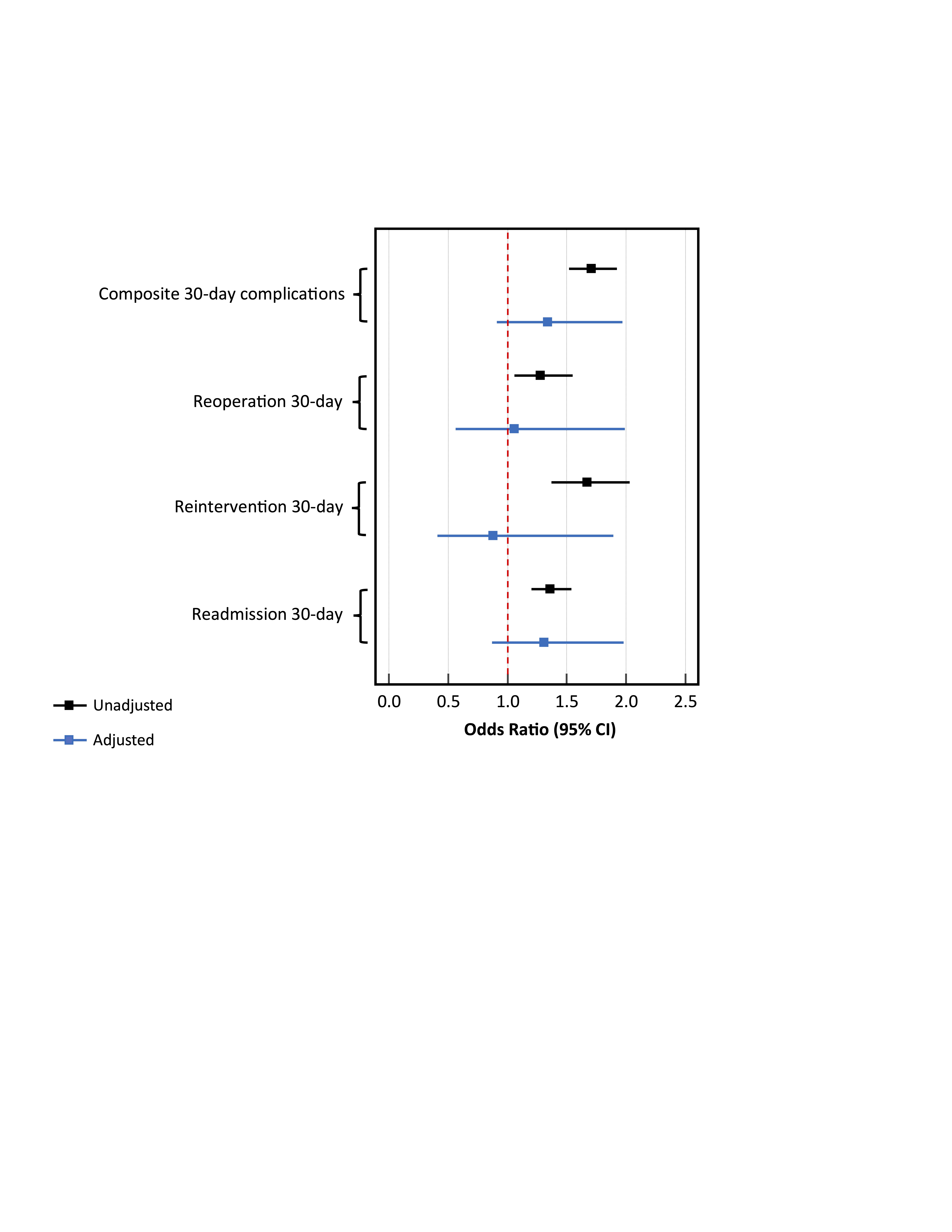
Figure 1. Univariate and multivariate regression analysis of albumin levels for predicting post-operative outcomes
Back to 2024 Abstracts


