Enteral nutrition is associated with high rates of pneumonia in intensive care unit (ICU) patients with acute pancreatitis
*Apostolos Gaitanidis, *Kerry Breen, *April Mendoza, *Noelle Saillant, *Jason Fawley, Haytham Kaafarani, *Jonathan Parks, George Velmahos, *Peter J Fagenholz
Massachusetts General Hospital, Boston, MA
Objective: Enteral nutrition is associated with improved outcomes in patients with acute pancreatitis (AP), but previous studies have not focused on critically-ill patients who may not tolerate enteral nutrition due to sedation or ileus. This study aims at determining the relationship between nutritional support used for AP patients in the ICU and subsequent infections.
Design: Retrospective cohort study
Setting: 127 hospitals participating in the eICU Collaborative
Participants: Patients with AP were identified and classified by the type (initial and any use) of nutritional support they received in the ICU: none (NN); oral (ON); enteral (EN); and parenteral (PN).
Main Outcome Measure: Infectious complications (pneumonia, bacteremia, sepsis/septic shock, pancreatic infection).
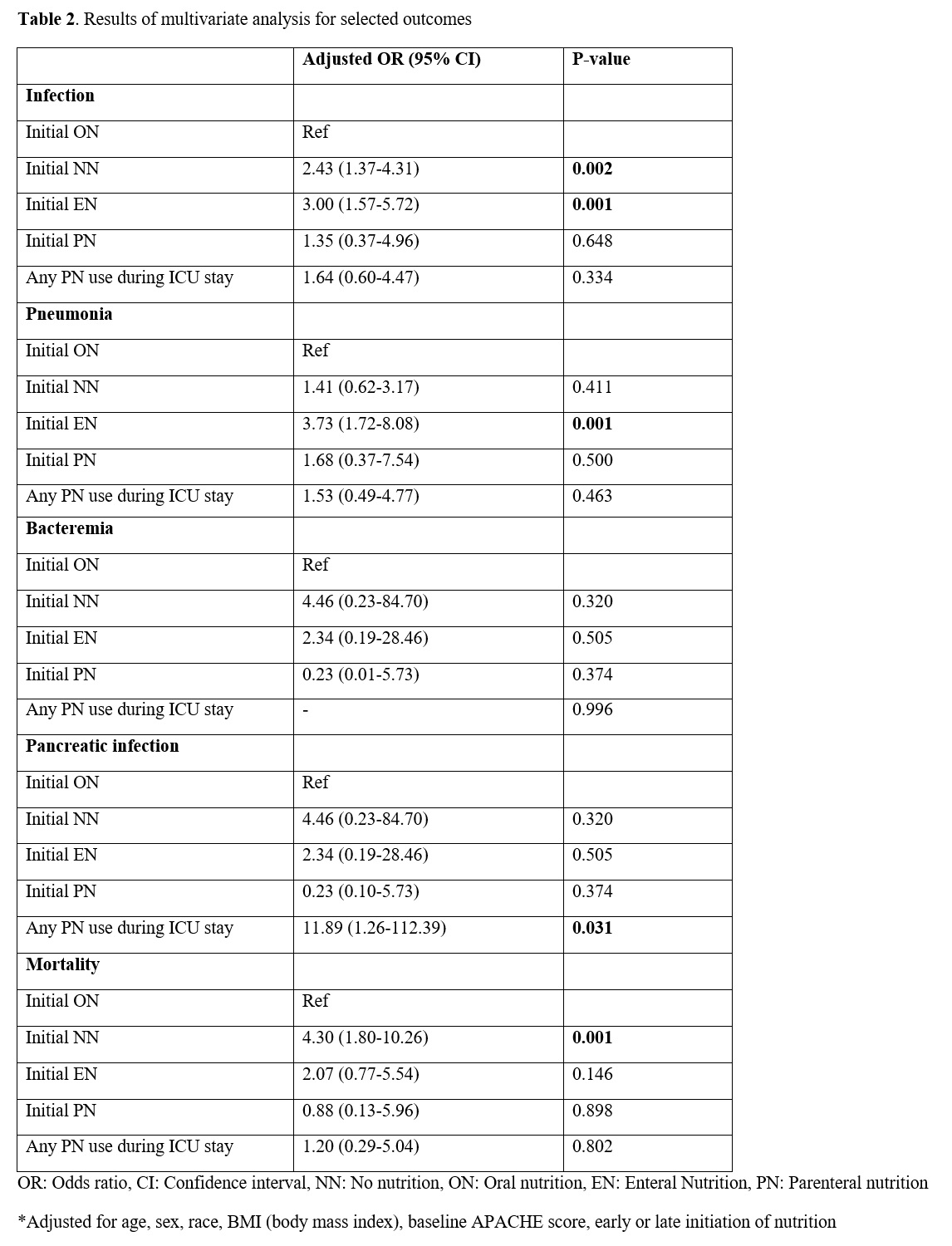
Results: 925 patients met inclusion criteria. 221 (23.9%) did not receive nutritional support (NN). Initial ON was used in 520 (56.2%), EN in 127 (13.7%) and PN in 57 (6.2%). Initial EN was associated with the highest rate of infectious complications (EN 28.4%, ON 6.9%, PN 21.1%, NN 14%, p<0.001), and pneumonias (EN 22.1%, ON 3.7%, PN 14%, NN 5%, p<0.001). Any PN use was associated with higher rates of pancreatic infections (PN 5.3%, EN 3.2%, ON 0.4%, NN 0.5%, p=0.001). These differences persisted in multivariate analyses adjusting for confounders (Figure 2).
Conclusion: PN is associated with higher rates of pancreatic infections in critically-ill AP patients. EN is associated with higher rates of pneumonia and overall infections. 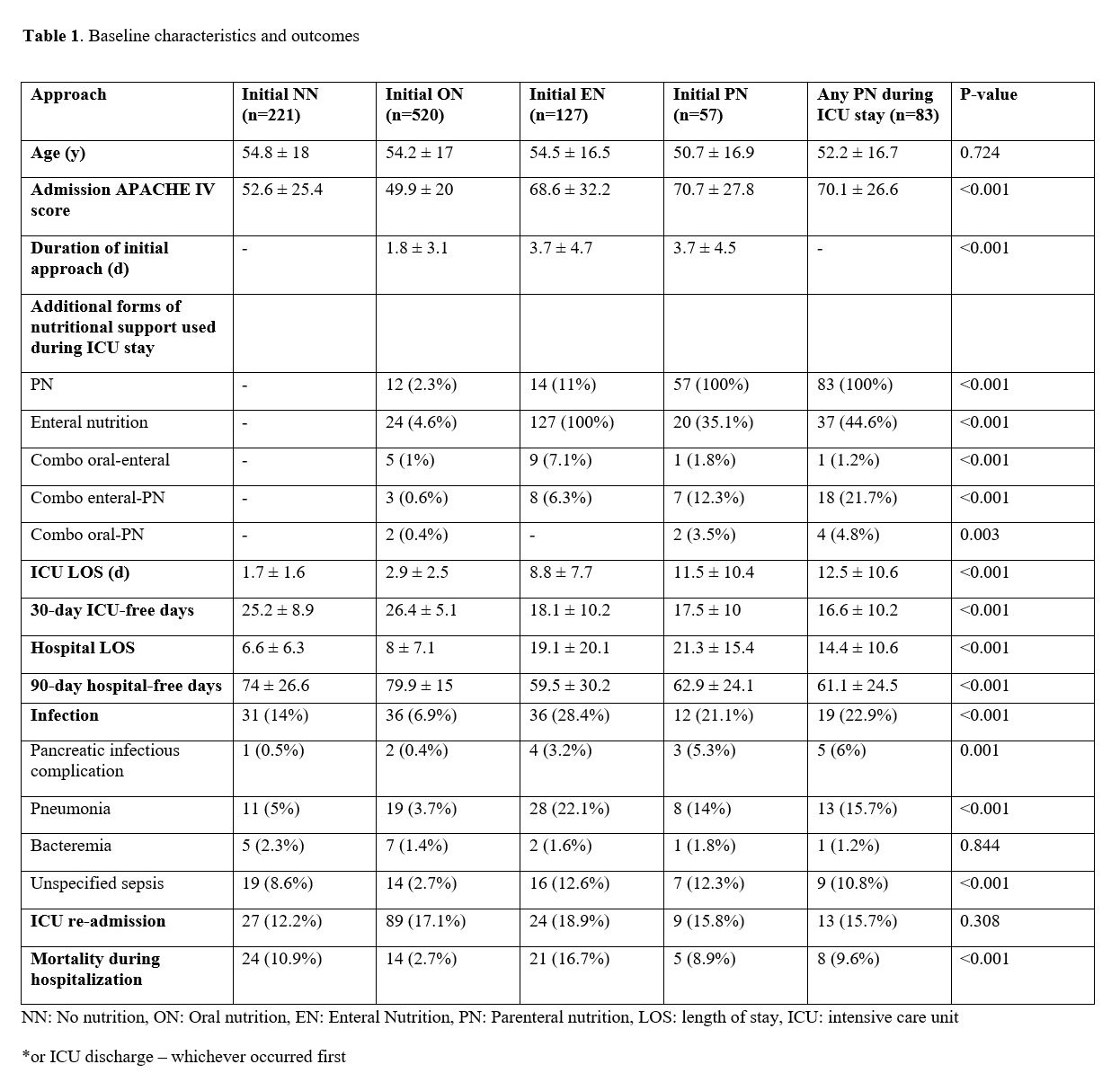
Back to 2020 Abstracts
