Back to 2025 Abstracts
An analysis of peritoneal aspirate – Examining the impacts of a 90-minute heated intraperitoneal chemoperfusion in patients with peritoneal malignancy.
Neelia E. Abadi
*Larner College of Medicine, University of Vermont Medical Center, Burlington, VT
Background: The acute effects of cytoreductive surgery with heated intraperitoneal chemotherapy (HIPEC) on the cellular environment remain poorly understood. This study assesses HIPEC’s impact during a standard 90-minute perfusion by quantifying cellular populations, with a particular focus on the immune cellular profile, in peritoneal aspirates from patients undergoing treatment.
Study Design: A biomarker-based translational approach was used. Over the course of each enrolled HIPEC, four aspirates (0, 30, 60, and 90 minutes) were collected from the hyperthermia pump used to lavage the peritoneum. Hemocytometry quantified viable and non-viable cells, while flow cytometry identified leukocyte subsets, including CD4 and CD8 T cells and CD19+ B cells.
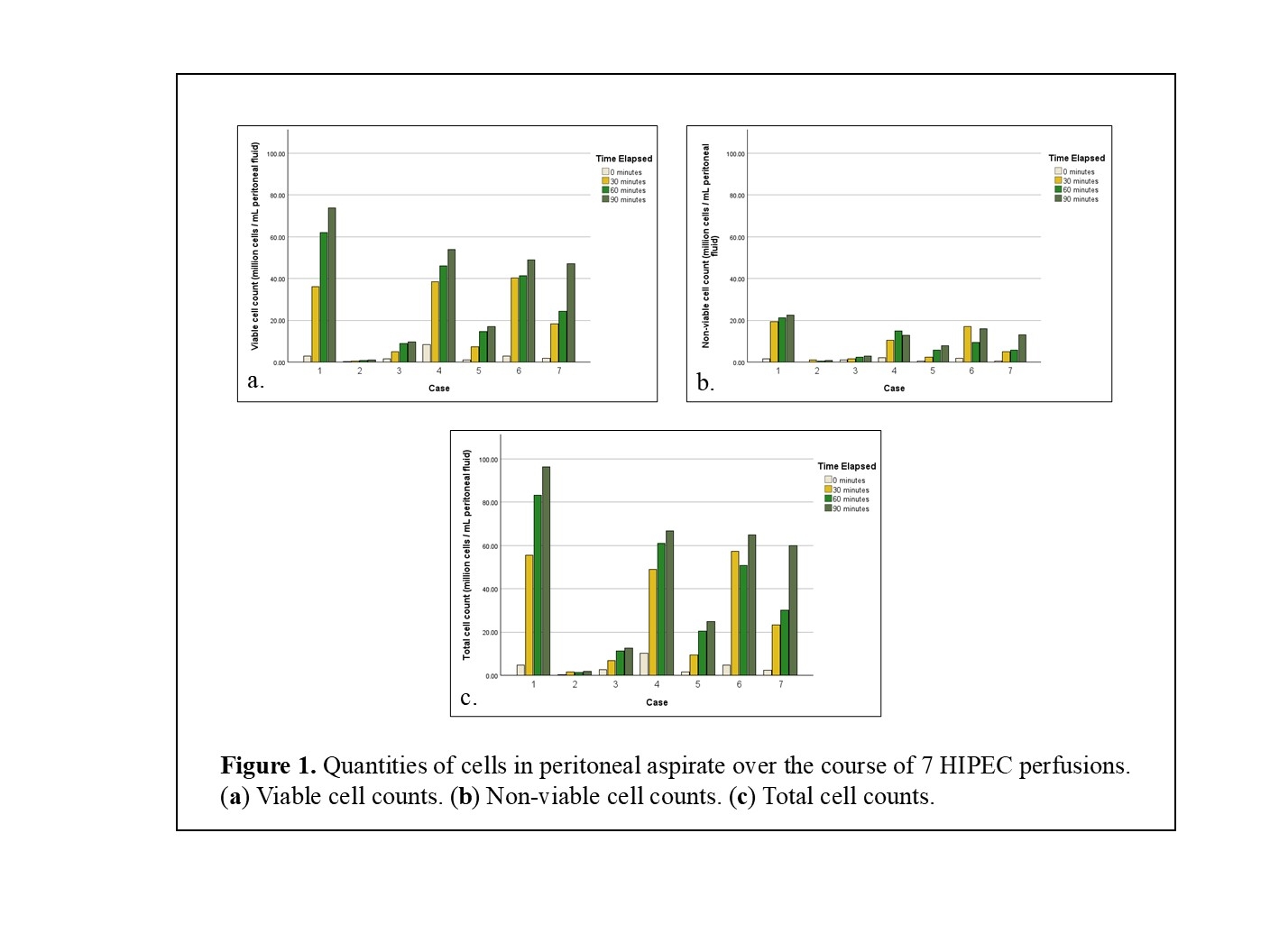
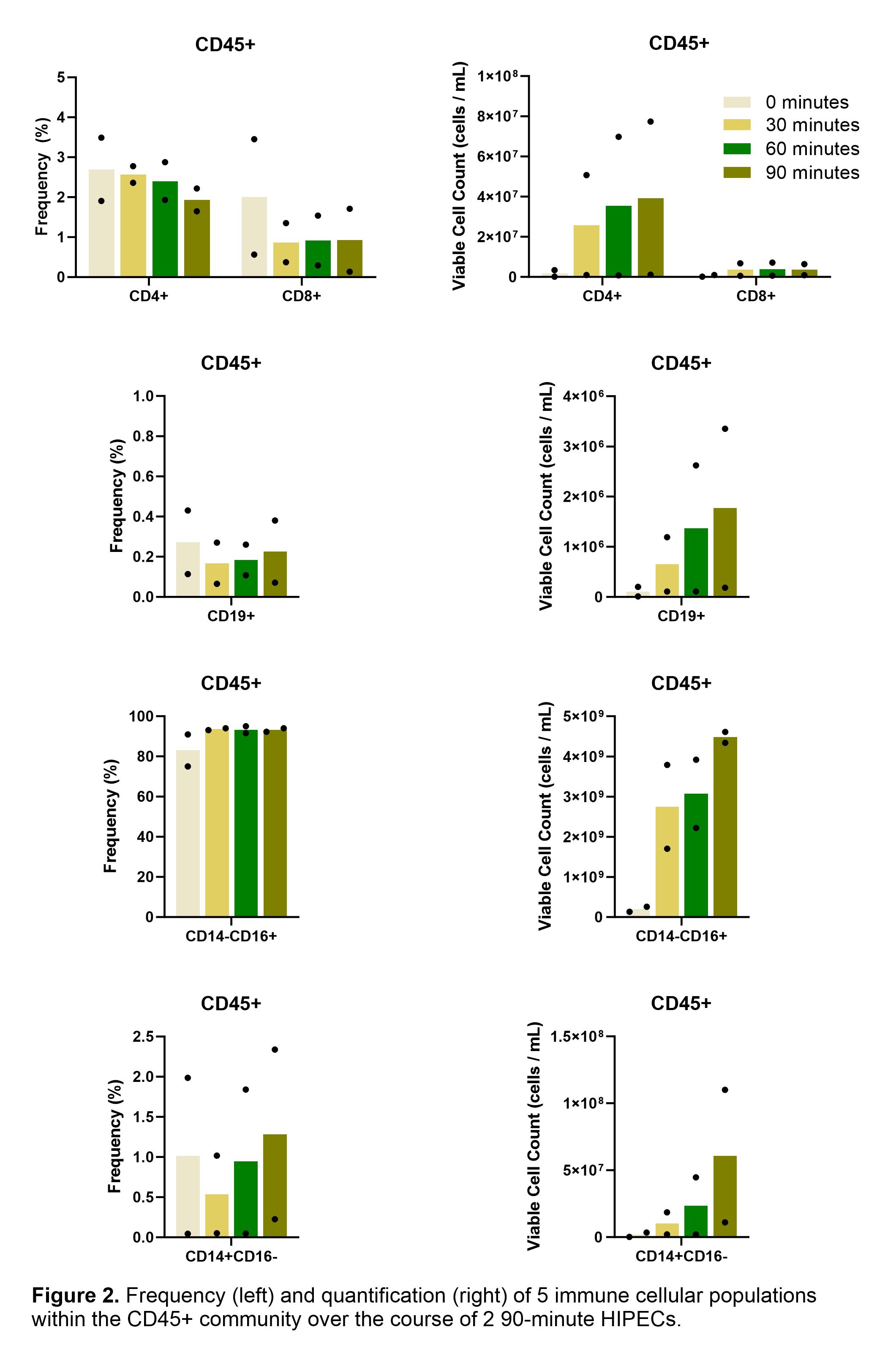
Results: Aspirates from seven participants over six months showed variable cell counts, ranging from 1.73 to 96.25 million cells/mL of peritoneal fluid at the 90-minute timepoint. Despite this variability in quantity, both total and viable cell counts showed a consistently positive trend over time. Across all six cases, the viable cell counts increased between each 30-minute interval, with overall percent change from 0 minutes ranging from 223.07% to 2358.33%. On average, the proportion of viable cells present was larger than that of non-viable cells at each time point. Flow cytometry was completed on samples from two participants, with the CD45+ antibody marking immune cells. At each time point, the dominant population of cells was found to be CD45+. Between 75.08% and 95.00% of CD45+ cells were identified as a CD14-/CD16+ myeloid population, associated with neutrophils. The proportion of CD4 T cells consistently exceeded that of CD8 T cells, while CD19+ B cells remained low (0.06%–0.43%). No trend in proportions of immune cell types was identified across time.
Conclusions: HIPEC acutely impacts the peritoneal environment, with a positive relationship between time in perfusion and the quantities of total and viable cells aspirated. Immune cells, specifically CD14-/CD16+ myelocytes, comprised the majority of this population. Characterizing the non-immune cells and comparing counts to patient blood panels can allow for the translation of these cellular impacts into clinical understanding.