Back to 2025 Abstracts
The Effect Of Bougie Size On Weight Reduction And Diabetes Remission Following Laparoscopic Sleeve Gastrectomy: A Single Academic Center Retrospective Cohort Study
Wasef Abu-Jaish
*, Elizabeth O'Neill, Keira Goodell, Susan Campbell
Surgery, The university of Vermont Medical Center. UVM College of Medicine., Burlington, VT
Introduction: Laparoscopic sleeve gastrectomy (LSG) is the most common bariatric procedure. We investigated which factors affect BMI reduction and diabetes mellitus (DM) remission following LSG.
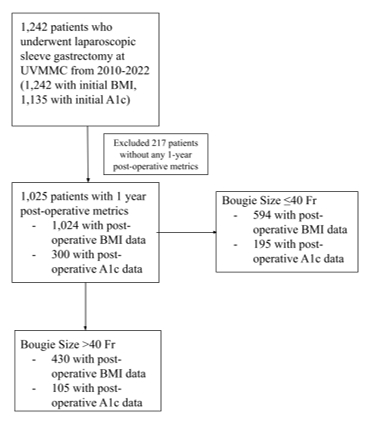
Methods: 1242 LSG patients from 2010-2022 were reviewed for demographics, pre-operative and one-year post-operative BMI, hemoglobin A1c, DM treatment, and bougie size (?40 Fr and >40 Fr). SAS was used for statistical analysis and two staple t-tests, paired t-tests, and ANOVA.
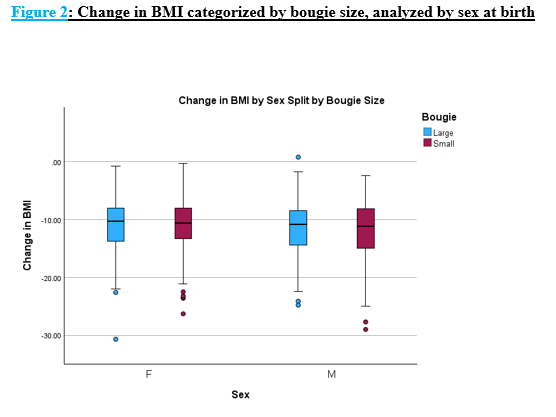
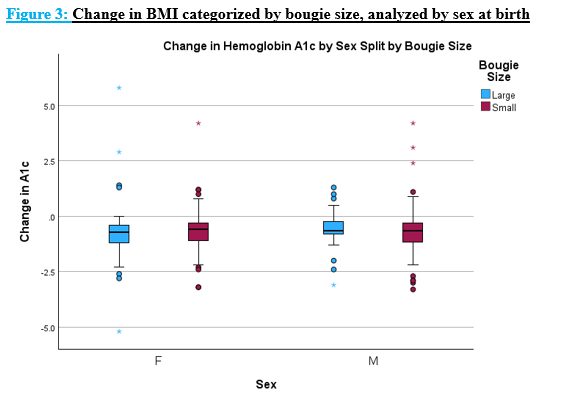
Results: Diabetic status: 44% non-diabetic; 25% pre-DM; and 31% Type 2 DM. Diabetic control: 17% diet-controlled; 29% insulin-dependent; and 54% oral antihyperglycemic (OA). Pre-operative DM had a significantly lower BMI reduction (9.39 � 4.34) compared to pre-DM patients (11.42 � 4.36) and nondiabetics (11.88 � 4.20) (p<0.001). BMI reduction did not significantly differ between pre-DM and the non-DM groups (p>0.05). Pre-op OA had a greater A1c reduction when compared to pre-op IDDM (0.8 � 1.1 compared to 0.4 � 1.0; p<0.007). There was no difference in BMI or hemoglobin A1c reduction when comparing sex or age. There was no significant difference between the mean BMI reduction between small (11.0�4.6) or large bougie (10.9�4.3) cohorts (p>0.05). There was no significant difference (p>0.05) in hemoglobin A1c reduction between small bougie (0.7�1.0) or large bougie (0.7�1.2) groups.
Conclusion: Non-diabetics had a significantly higher weight loss when compared to diabetics, regardless of control agent. IDDM was associated with the least BMI and A1c reduction. Bougie size did not affect measured outcomes. This data suggests that pre-operative factors of modifiable factors should remain a mainstay in all bariatric programs.
Demographics
| | Small (?40 Fr) | Large (<40 Fr) |
| Variable | Mean | Std | Mean | Std |
Age at time of surgery
Pre-Op BMI
Pre-Op A1c | 46.1
44.4
6.75 | 11.3
6.7
0.9 | 44.3
44.1
6.86 | 10.7
6.2
0.9 |
| | n | % | n | % |
Sex
F
M | 466
128 | 78.5
21.5 | 341
89 | 79.3
20.7 |
Diabetes Status
No
Pre-Dm
Diabetes | 4
38
152 | 2.1
19.5
78.5 | 5
14
86 | 4.8
13.3
81.9 |
Age
20-34
35-44
45-54
55-64
65+ | 112
163
166
123
30 | 18.9
27.4
27.9
20.7
5.1 | 90
132
124
72
12 | 20.9
30.7
28.8
16.7
2.8 |