Back to 2025 Abstracts
Post-Operative Adverse Events and the Area Deprivation Index after Sleeve Gastrectomy
Daniel Uzochukwu
*, Ali A. Nimeri, Marcus McKenzie, Zachary Ballinger, Obinnaya Okereke, Katharine P. Playter, AbdulAziz Khan, Banafo Abbeyquaye, Richard A. Perugini
UMass Chan Medical School, Worcester, MA
Background: The Area Deprivation Index (ADI) is a validated tool that accurately represents socioeconomic disadvantage status using income, education, and employment. High ADI can have a significant impact on a patient's ability to recover from surgeries and their likelihood of having surgical complications. The relationship between ADI and postoperative outcomes in sleeve gastrectomy (SG) has yet to be studied. We aim to investigate ADI and postoperative adverse events after sleeve gastrectomy to better understand the impact of socioeconomic factors on recovery and complications.
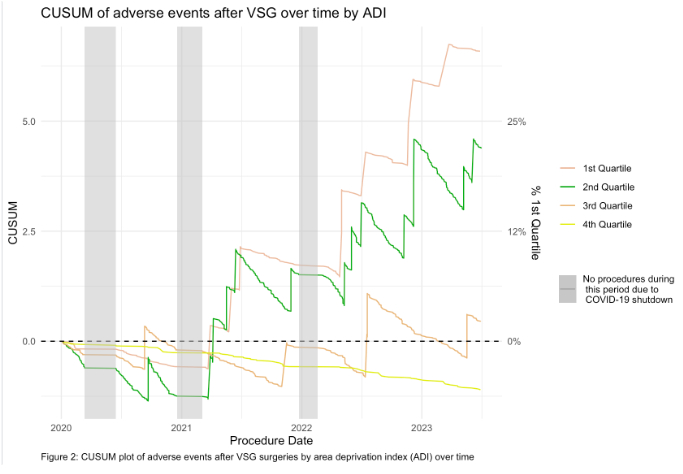
Methods: This retrospective cohort study included patients who underwent SG between January 2020 and December 2024. Adverse events were defined by MBSAQIP registry criteria. ADI national percentile and state decile were determined. Temporal trends of adverse events following sleeve gastrectomy were studied using cumulative summation (CUSUM). Univariate and multivariate analyses were carried out to identify factors predictive of adverse events.
Results: In total 1483 patients had SG during the study period. The rate of adverse events after SG was 2.3% (n=33). Hemorrhage accounted for 48% of adverse events after SG. The rates of postoperative adverse events decreased with increasing ADI national quartile (Q1: 4.8%, Q2: 2.2%, Q3: 1.6%, Q4: 0%). 5th ADI national quintile patients had a significant reduction in risk of adverse events when compared to 1st quintile patients on univariate logistic regression (OR: 0.26 95% CI: 0.07-0.90, p= 0.03). For every 1-point increase in ADI rank (State or National), the odds of an adverse event were reduced by 3% in models controlling for demographics, comorbidities, and operations during and after the COVID-19 pandemic (OR: 0.97, CI: 0.94-0.99, p: 0.012) (Table1).
Conclusion: Surprisingly, increasing deprivation as assessed by ADI was found to have an inverse relationship with the risk of adverse events. This unexpected finding may be due to a rigorous selection process for SG candidates and may be specific to metabolic/bariatric surgery. Further studies will need to be done in other centers to corroborate this finding.
Multivariable Logistic Model of Adverse Postoperative Events
| Variable | Odds Ratio | 95% confidence interval | 95% confidence interval | p-value |
| Robotic Approach | 0.472 | 0.223 | 1.00 | 0.051 |
| Tri-date Period: | | | | |
| Between January, 2021 and May 11, 2023 | 5.37 | 1.19 | 24.1 | 0.028 |
| After May 11, 2023 | 5.7 | 1.09 | 29.87 | 0.039 |
| ADI National Rank | 0.966 | 0.940 | 0.992 | 0.012 |