Assessing Cost-Effectiveness of Admission and Interval Imaging to Improve Outcome After Delayed Traumatic Intracranial Hemorrhage: a Decision-Analytical Model
*Norman G. Nicolson, Kevin Y. Pei
Yale School of Medicine, Department of Surgery, New Haven, CT
Objective: Delayed intracranial hemorrhage (dICH) among patients on anticoagulation is a rare, but potentially lethal complication after blunt trauma. Although some guidelines recommend repeat imaging and an observation period, a recent study showed that these events may occur in only 1.3% of therapeutically anticoagulated trauma patients. We hypothesize that although individual patients may occasionally benefit from the practice, admitting for observation and repeat scan is not cost-effective.
Design: Cost-effectiveness analysis through a decision-analytical model
Setting: Emergency department
Patients (or Other Participants): Patients aged 40-80, after a fall on anticoagulation, with normal initial head CT
Interventions: Admission and interval imaging, versus discharge from the emergency department
Main Outcome Measures: Expected costs (2017 US$) and quality-adjusted life-years (QALY)
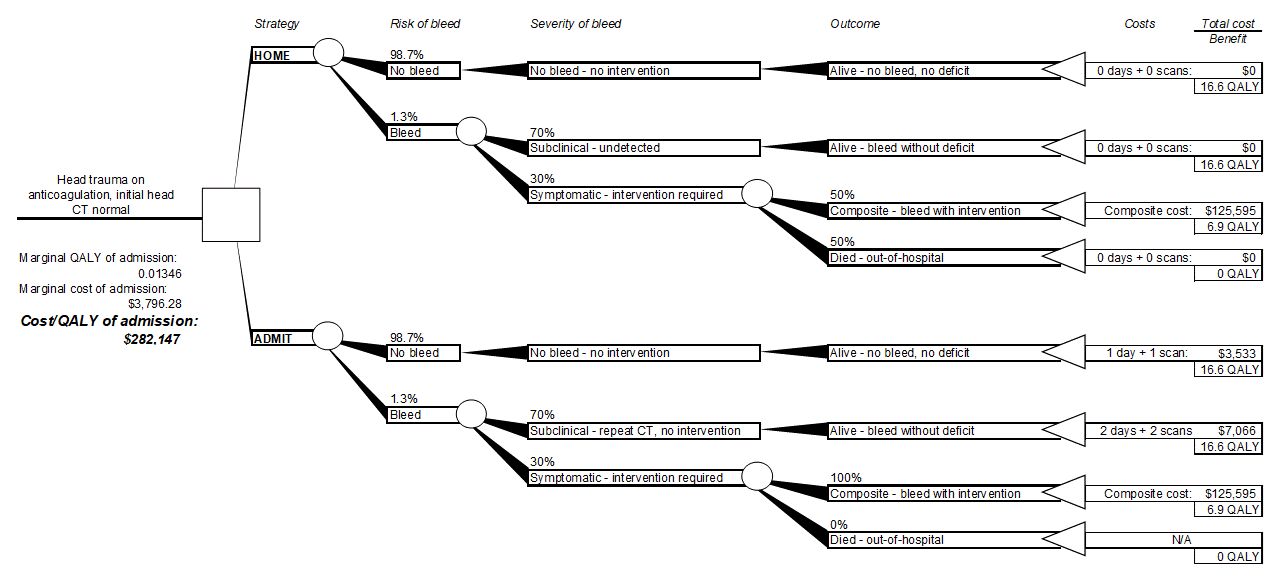
Results: Under the default assumptions, the incremental cost of one QALY for admission was $282,147. Sensitivity analysis revealed a range of $66,978/QALY (if the dICH rate was 7.2%, the upper limit in the literature) to $13,215,421/QALY (if only 1% of discharged patients with major dICH requiring neurosurgical care died pre-hospital).
Conclusions: For patients presenting to the emergency department after blunt trauma with initially normal cross-sectional brain imaging, admission for observation and repeat imaging is not cost-effective at the usual threshold of ,000/QALY, even for anticoagulated patients. In an environment of scrutiny on high-cost/low-benefit interventions, these admissions are likely an avoidable source of medical resource utilization.