Implementation of Enhanced Recovery After Surgery Decreases the Length of Stay Following Living Kidney Donor Nephrectomy
Nahel Elias, *Jennifer MacCready, *Laura Rossi, Tatsuo Kawai
Massachusetts General Hospital, Boston, MA
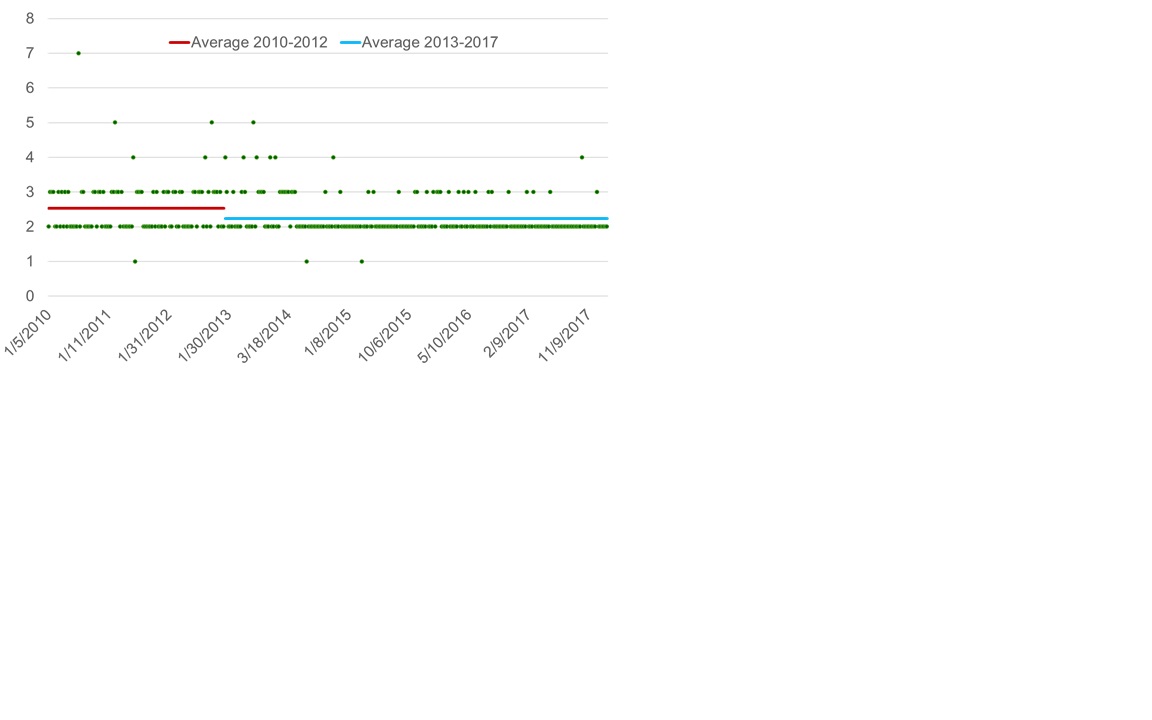
Objective(s): Evaluation of Enhanced Recovery after Surgery (ERAS) protocol on length of stay (LOS) and readmission of Living kidney donors (LKD) Design: Non-randomized intervention study with historic control. The study was initiated in January 2013 and continued through December 2017. The control group were the prior LKD performed in 2010-2012. Setting: A tertiary referral hospital, with experience in laparoscopic living donor nephrectomy and kidney transplantation. Patients: LKD are healthy volunteers, who undergo nephrectomy to provide an important treatment option to benefit patients with end-stage renal disease. The intervention included 231 LKD: 76 men; 155 women (age range 21-73), the control group was 106 LKD: 39 men and 67 women (age range 21-66). All LKD performed at our center were included in the study. Interventions: A multidisciplinary transplant team developed and introduced a new ERAS-like pathway. The revised pathway included: 1) Preoperative bowel regimen 2) Postoperative plan for activity progression and 3) Pain management protocol. A peripheral nerve block was placed in the OR followed by IV patient-controlled analgesia. On POD 1, Foley catheter was removed; oral pain management and ambulation were initiated. Main Outcome Measure(s): LOS and readmission rates Results: The mean LOS (standard deviation) for LKD between 2007-2012: 2.53 (0.78); between 2013-2017: 2.24 (0.54) which was statistically significant P=0.0009. An analysis of 30, 60, 90-day readmission rates remained unchanged. Conclusions: Implementation of a standardized pathway is effective in reducing LOS for LKD without affecting readmission rates. Improved pain management with early ambulation appears to have the greatest influence.
Back to 2018 Program




