Outcomes of extended lymphadenectomy (LAD) for gastroesophageal carcinoma (GEC): A large Western series
*Selena Li1, *Christina L Costantino2, David W Rattner2, John T Mullen2
1Harvard Medical School, Boston, MA;2Massachusetts General Hospital, Boston, MA
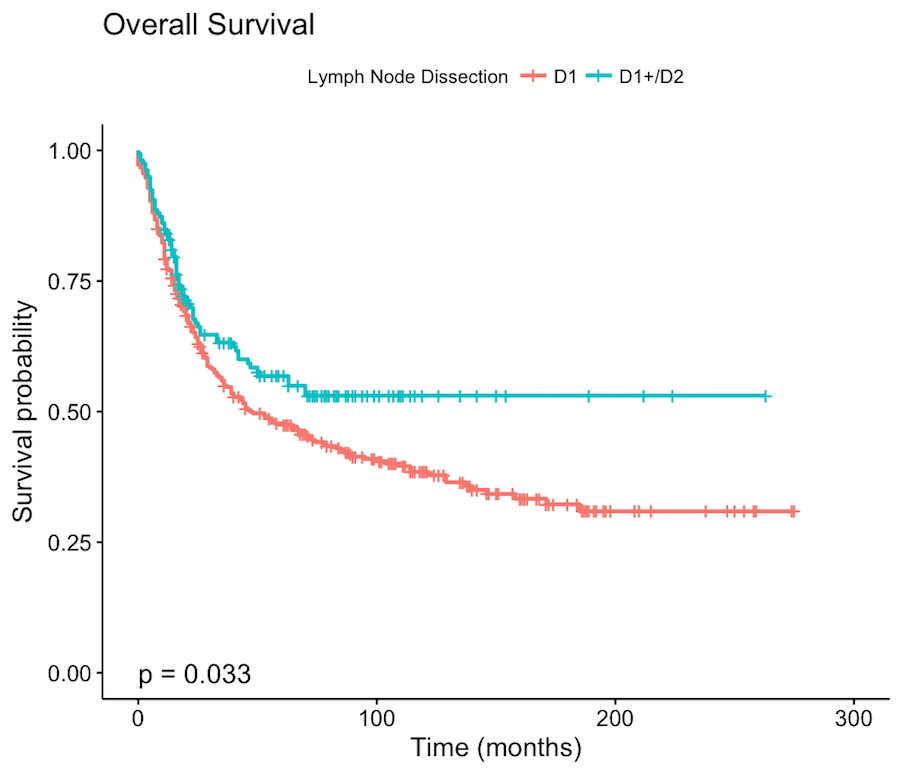
Objective: To examine perioperative risk and survival outcomes in a large Western series of patients undergoing D1 versus extended (D1+/D2) LAD for GEC. Design: Single institution, retrospective chart review. Clinicopathologic and treatment factors were analyzed for their impact on survival by univariate and multivariate regression analyses. Setting: Academic medical center. Patients: 520 patients with GEC who underwent potentially curative gastrectomy from 1995-2017, including 362 (70%) patients undergoing D1 LAD and 158 (30%) undergoing D1+/D2 LAD. Interventions: None Main Outcome Measures: Perioperative morbidity and mortality, lymph node yield, and overall survival. Results: Median follow up was 3.1 years. Patients undergoing D1+/D2 LAD were more likely to have distal tumors, to undergo distal/subtotal or total gastrectomy, and to undergo surgery at a more contemporary time (median year 2011 versus 2006) than patients undergoing D1 LAD. The median number and percentage of patients with >16 examined lymph nodes were 16 and 53% versus 27 and 89% in the D1 and D1+/D2 groups. There were no differences in the rates of major complications (16.6% versus 14.6%; p>0.05) or operative mortality (2.8% vs 0.6%; p=0.22) between the D1 and D1+/D2 groups, respectively. Patients undergoing D1+/D2 LAD had a significantly improved overall survival (HR 0.67, p=0.013) on multivariate analysis compared to those undergoing D1 LAD (Figure), though there were several potential unmeasured confounding variables. Conclusion: Gastrectomy with extended (D1+/D2) LAD can be safely performed at a high-volume Western institution, ensures optimal staging in the vast majority of patients, and may confer a survival advantage.
Back to 2018 Program




